Maintaining good dental health is about more than having an attractive smile. Problems with your teeth and gums can lead to serious, and even life-threatening, issues with your cardiovascular system and respiratory system. Thankfully, non-surgical gum disease treatments can correct gum[…]
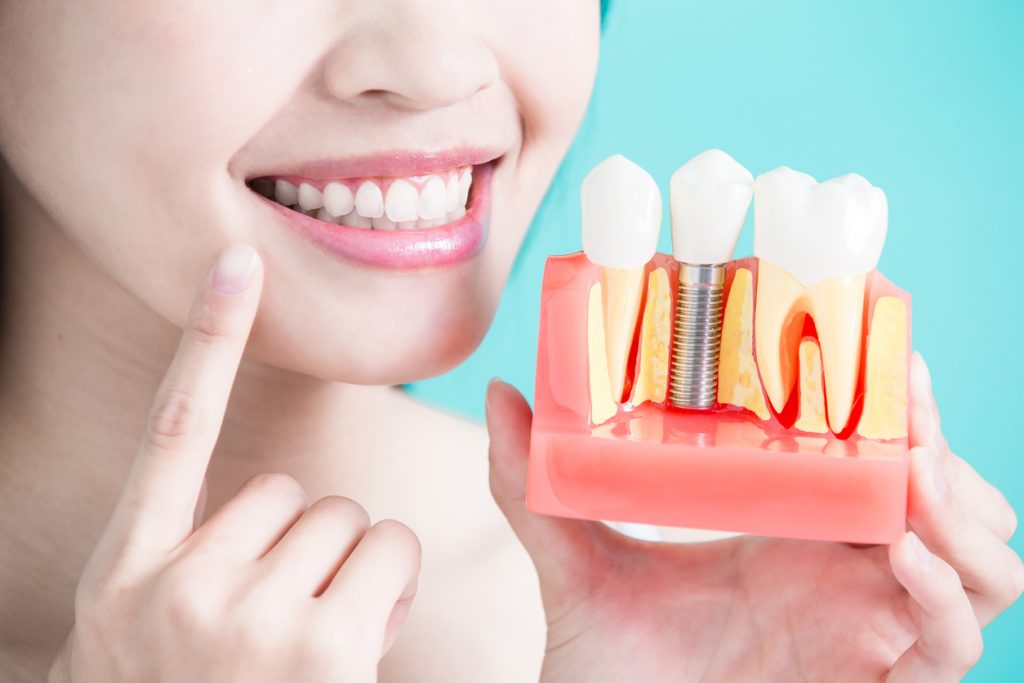
Are Dental Implants Safe?
If you have suffered the loss of one or more teeth, a dental implant is the most natural way to replace them. Unlike a bridge, which attaches to surrounding teeth and fills the gap, or a crown, which replaces only[…]
How to Prevent Periodontal (Gum) Disease
If you don’t maintain good dental hygiene, bacterial growth in your mouth can lead to periodontal (or gum) disease. Your gums might bleed or recede from your teeth, requiring early intervention. Gum disease is reversible if you catch it soon[…]
Comparing Dental Implants, Dental Bridges and Dentures
Dental technology has come a long way in recent years, and there are now a number of options when it comes to dealing with one or more missing teeth. Patients can now choose between custom-made removable dentures, a dental bridge,[…]
AZ Periodontist: How Dr. Trujillo Can Help
How can an AZ periodontist help? Understanding this allows you to seek the necessary dental treatment you may need. A periodontist is an expert specializing in preventing, diagnosing, and treating diseases and conditions, impacting your teeth’ supporting tissues such as[…]
Sensitive Teeth Treatment
Do you experience discomfort or pain in your teeth when eating ice cream or something cold or hot? If so, you probably have teeth sensitivity. When your teeth are sensitive, activities like drinking, eating, and brushing can cause your teeth[…]
Discover the Secret of Affordable Dental Implants in Phoenix, AZ
Updated: 7/2023 How much is your smile worth to you? When it comes to the cost of dental implants, some people feel like they have to decide between their smile and their bank account. For those without dental insurance, the[…]
Gum Grafting: Procedure and Aftercare
Gum grafting is a dental procedure to fortify areas of the mouth that lack gum tissue by adding new layers of tissue. This material typically comes from another section of the patient’s mouth, which is numbed beforehand. The purpose of gum[…]
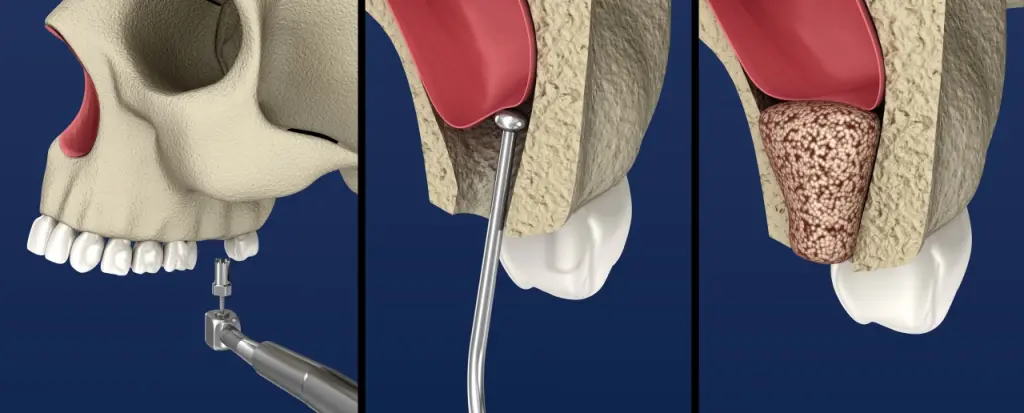
Sinus Lift: What It Is and Why You May Need It
Dental implants are ideal for patients who have one or more missing teeth. Recent studies reveal that there are about 5 million implant procedures done by dentists in the United States annually. Some situations may require additional treatments before an implant can[…]
Gum Whitening: Benefits and Candidates
While discoloration on your gums is usually harmless, it can negatively impact self-confidence and make you reluctant to smile. For this reason, many patients undergo gum whitening, a cosmetic procedure to remove dark spots to enhance the appearance of their[…]